Eye Health
Home » Keratoconus
Blurred vision is a common symptom of several conditions. Finding out which condition is causing yours can be equally difficult. The first step is eliminating other simpler conditions before moving to the bigger ones. Your doctor may first check your prescription to see if your prescription has changed then other options can be evaluated.
Keratoconus can cause your vision to worsen over time and if your prescription continues to change it is possible you may have Keratoconus. It is also important to know your family history so you know whether to eliminate that option right away.
Below you will see some symptoms of Keratoconus:
Blurred vision
Frequent Prescription changes
Sensitivity to light
Poor night vision
Headaches
Straining of the eyes
Sudden Cloudiness in your vision
If you have symptoms like those listed above speak to your eye care professional right away as Keratoconus can worsen very quickly. For additional questions on Keratoconus please call our office at (310) 860-1900.
Keratoconus is a progressive eye disease that may worsen over time if it is not treated. If you are noticing that your eye prescription is constantly changing, the first step would be visiting your local eye doctor. Frequent changes in prescription may be a sign of Keratoconus and possibly a sign of more serious conditions. If Keratoconus runs in your family, it does not necessarily guarantee that you will get it, but it does put you more at risk. Below are some signs and symptoms of Keratoconus.
This site discusses Keratoconus treatments that can help you. Treatments include Holcomb C3-R, Intacs, Ck and Visian ICL.
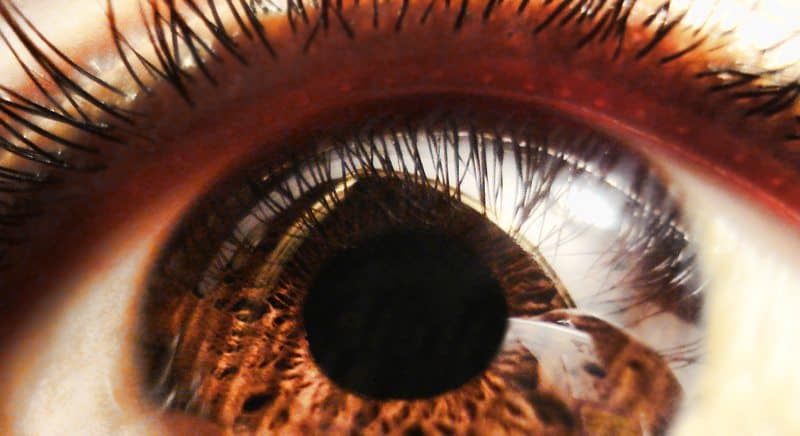
Below are some early signs
Today’s Keratoconus treatment options have been effective in reversing and stopping the worsening. The Holcomb C3-R® invented by Dr. Brian, is the first non-invasive corneal crosslinking procedure for Keratoconus, which has the longest track record of any form of crosslinking in the world (except Germany). Another procedure that is often combined with the Holcomb C3-R® is Intacs® which are clear tiny semi-circles that are placed in the cornea to help reshape the cornea. Dr. Brian pioneered Intacs® for Keratoconus in 1999 and has the longest experience in the world with it for Keratoconus- 18 years.
If you have been experiencing any of these signs and symptoms, make an appointment with our office today to be considered for a Holcomb C3-R® evaluation. Please call (310) 860-1900 or email us at Info@boxerwachler.com
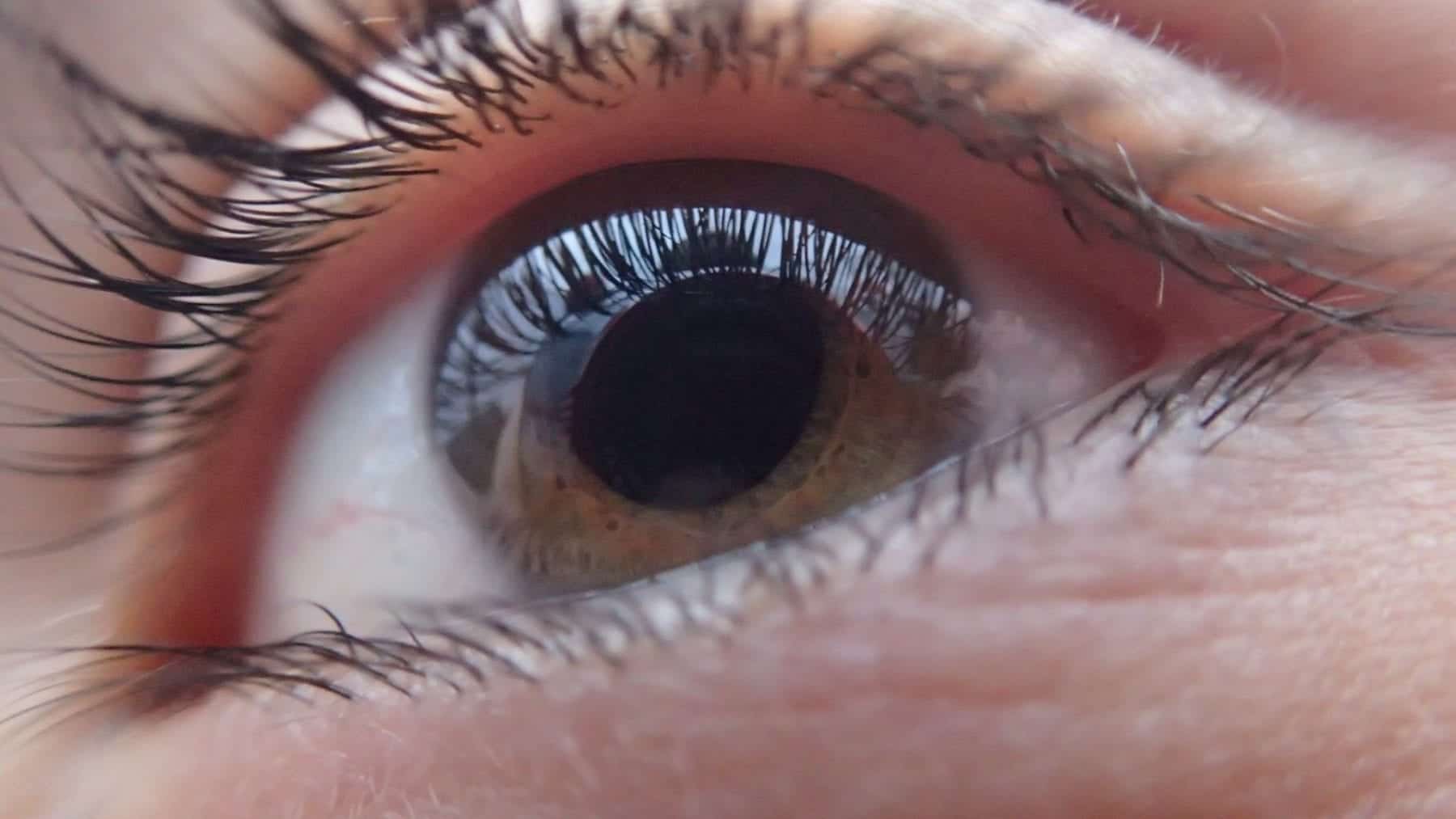
Holcomb C3-R ®
Holcomb C3-R ® has been available since 2003. This procedure helps improve the strength of the weakened cornea fibers. It is a non-invasive procedure that works over 4-16 weeks to improve strengthen the cornea fibers. The Holcomb C3-R ® can be done on the same day as several other treatments like Intacs®, CK, or even PRK.
Intacs®
Intacs® is a procedure in which a tiny crescent shaped lens inserts are placed the layer of the cornea to help improve the shape and decrease the irregular cornea shape. This procedure can be done in combination with the Holcomb C3-R ® providing improvement in your quality of vision. It only takes 7 minutes to complete and it is showing great promise in the treatment of Keratoconus.
CK or Conductive Keratoplasty
CK uses radio frequency to reshape the cornea. This treatment improves the curves of the cornea, which can improve the overall vision. There is little to no pain during the procedure and it only takes around 3 minutes to complete. This treatment can be combined with the Holcomb C3-R ® or Intacs® and can provide improved outcome for reducing high amounts of astigmatism.
Benefits of Combining Treatments:
• Improved Vision Outcomes
• Less Recovery Time – only 1 day of procedures, rather than multiple days
• Faster Results
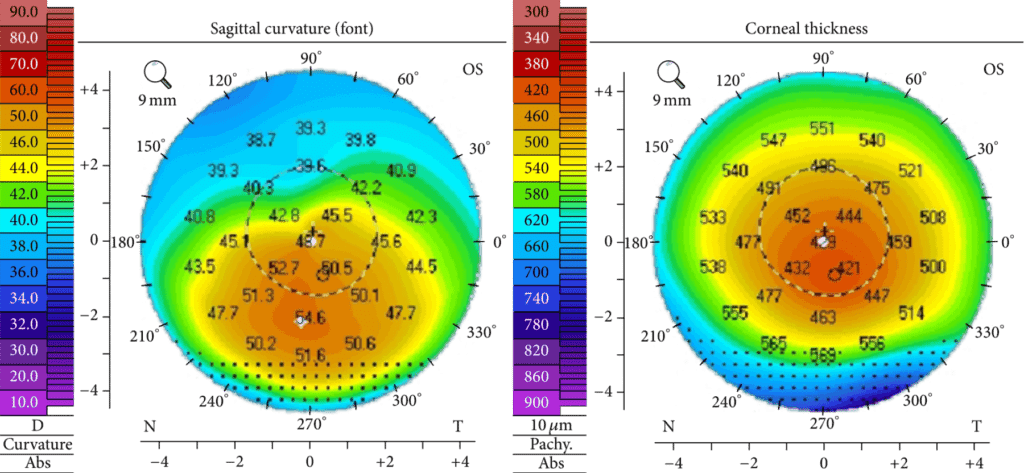
Many cornea transplant surgeons whose practice is based on performing corneal transplants, want you to think this is the only option. They do not want you to know that there is an alternative non- invasive crosslinking procedure called Holcomb C3-R. Invented in 2003, this crosslinking procedure has the longest track record of any form of crosslinking in the United States.
Intacs do not “float around.” They are tiny semi-circle inserts that are placed in the peripheral layer of the cornea. They are immediately locked in place and sealed by the “healing process,” and patients usually do not feel them. Dr. Brian pioneered Intacs in 1999 and has had the longest experience in the world doing so.
Intacs do not wear out or degrade and do not need to be replaced.
Contact lenses are often mistaken for stopping the worsening of Keratoconus, but the truth is no contact lens is able to stop or slow down the worsening. The main purpose of contacts is to “smooth out” the eyes surface while improving the vision. There are six different types of custom lenses that are a possible fit for a patient. Fitting for Keratoconus patients can be difficult, because the lens must fit around the cornea’s bulge, while still maintaining the comfort and proper fit, but it is nothing Dr. Weiss, Keratoconus contact lens specialist can’t help you with.
Most people diagnosed with Keratoconus are under the age of 30 years old, but there are a number of patients who get diagnosed that are in their 40’s and even 50’s. Although age does not play an important factor because anybody could be diagnosed, Keratoconus occurs in 1 in 500 people.
Often times Keratoconus patients with severe cases are told by their doctors that their only options are an invasive cornea transplant or hard contact lens. Dr. Boxer Wachler has made the technological advances to help people who could not be helped in the past, leaving patients with a peace of mind.
Is it difficult for you to see while driving at night? Do you have to strain to see the street signs? How well can you see the traffic lights or other cars on the road? Millions of people suffer from difficulties driving during the night, it is called Night Blindness and there are treatments.
What is Night Blindness?
Night Blindness or Nyctalopia is when a person has difficulty seeing at night or it becomes impossible to see in the dark. Night blindness is often a symptom of certain medical or vision conditions. Often patients with night blindness can not participate in normal activities at night or in the dark.
What are the Causes of Nyctalopia?
Nyctalopia or night blindness is often a symptom of certain medical or vision conditions. Many include Cataracts, Macular degeneration, Retina Detachment, Diabetes, and even Keratoconus. But you can also have Nyctalopia at birth, through injury, or from malnutrition or lack of vitamin A (Retinol).
What are the Symptoms of Nyctalopia?
What are the Treatments for Night Blindness?
When it comes to treatment options for those who suffer with Night blindness largely depends on the overall cause of the onset. Treatment options can include everything from a simple change in the patients eye glass prescription, to a change in medication. In some cases the patient may need surgery if the symptom creates too many complications.
Night blindness can be a very difficult symptom but with the help of your eye care professionals you can get help.
Keratoconus occurs in 1 in 500 people. Studies suggest that the weakening of the eyes corneal tissue may be caused by the imbalance of enzymes in the cornea which causes the cornea to bulge into a football shape instead of its natural rounded shape. Keratoconus is also said to be linked with overexposure of ultraviolet sun rays, eye rubbing and poorly fitted contact lenses. Other studies suggest that keratoconus is linked with hereditary predispositions as either a dominant or recessive trait. If you are having keratoconus symptoms it is important to review your families eye history. Below are some symptoms to help you detect the early stages of Keratoconus.
Your vision is an essential part of living a normal life. When it comes to your eyes, detecting early symptoms of Keratoconus is important. Knowing your family history and scheduling regular eye exams can help you with the diagnosis of the condition before it worsens. If the condition is left untreated it can cause difficulty driving at night, while decreasing the ability to see well with glasses or contacts. Below is a list of signs and symptoms.
• Blurred vision
• Glasses or Contacts do not improve the vision
• Frequent rubbing of the eyes
• Prescription changes
• Halos or glare around lights
• Decreased night vision
Treatments for Keratoconus
• Holcomb C3-R Cornea Collagen Crosslinking
• Intacs
• CK for Keratoconus
• Visian ICL
Since 1999 Dr. Brian Boxer Wachler, expert in Keratoconus Treatments has been treating patients from all over the world every week. Early detection can slow the progression of your Keratoconus while saving and preserving your vision. Call our office today to schedule an appointment at (310) 860-1900.